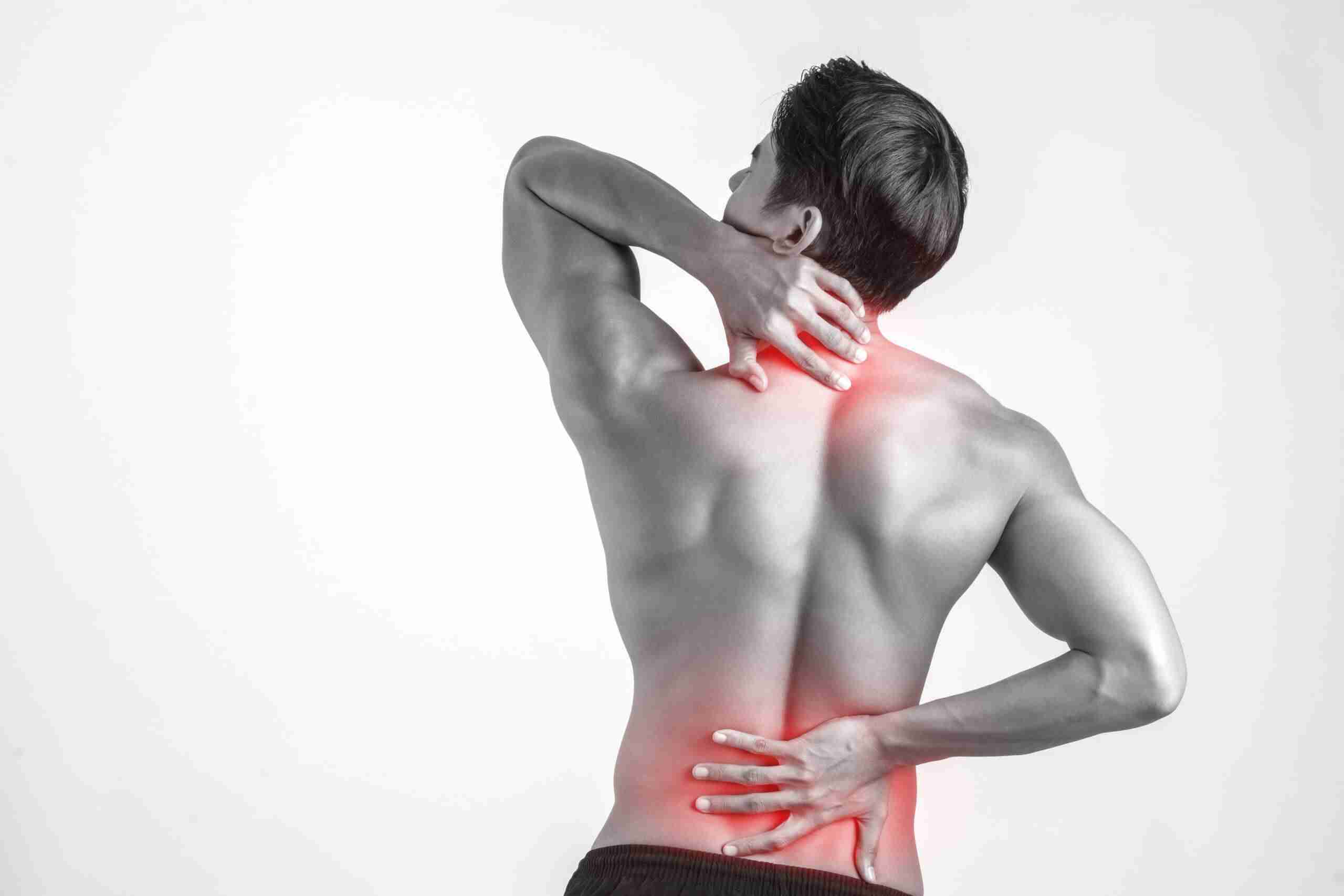
Lumbar radiculopathy, also known as sciatica, is a condition characterized by pain, weakness, and numbness that radiates from the lower back down the leg. It is caused by compression or irritation of the nerve roots as they exit the lumbar spine. The condition can be caused by a variety of factors, such as a herniated disc, degenerative disc disease, or spinal stenosis.
What is lumbar radiculopathy?
Lumbosacral radiculopathy is a pain syndrome that happens when nerve roots in the lower back are pinched or irritated. It can be caused by a herniated lumbar disc, degeneration of the vertebrae, or a narrowing of the foramen, the opening where the nerves leave the spinal canal. The pain usually goes in the direction of the involved dermatome in the leg. This is the area of the leg that the specific nerve covers. When a nerve at the L4-5 or L5-S1 level (the two lowest levels) is affected, the sciatic nerve, which runs down the back of each leg to the foot, is usually the dermatome.
Radicular pain can also be accompanied by numbness, tingling, muscle weakness, and the loss of specific reflexes. “Radiculopathy” is the name for nerve damage that shows up in the form of symptoms.
What issues does Lumbar Radiculopathy lead to?
Some people with radiculopathy also have myelopathy, which is when the spinal cord is compressed. When a disc is herniated or bulging, it can put pressure on the spinal cord and nerve roots. When the spinal cord is affected, the symptoms can worsen, including poor coordination, trouble walking, and even paralysis.
Lumbar Radiculopathy Symptoms
- sharp pain started in the back.
- sharp pain with sitting or coughing.
- numbness or weakness in the legs and feet.
- numbness or tingling in the legs or feet
- sensation or reflex changes, hypersensitivity.
Symptoms include low back pain that radiates into the lower extremities in a dermatomal pattern. Lumbar radiculopathy can also cause numbness, weakness, and loss of reflexes, but not having these symptoms doesn’t mean you don’t have it.
Treatment for Lumbar Radiculopathy
Most of the time, non-surgical treatments, like physical therapy, medications, and selective spinal injections, are recommended to last six to eight weeks. If nonsurgical treatment doesn’t help relieve the pain, decompressive surgery, such as laminectomy and/or discectomy/microdiscectomy, may be suggested.
This type of surgery usually helps 85 to 90 percent of patients with radicular pain or leg pain. After six weeks of non-surgical treatment, Lumbar Radiculopathy may suggest this surgery for people with severe leg pain or other serious symptoms like getting weaker over time. Back surgery to treat radicular pain (pain in the legs) is much more likely to work than the same surgery to treat low back pain.
Typically, radiculopathy is treatable without surgery. Depending on the severity, a doctor may recommend medication, including
- non-steroidal drugs, such as ibuprofen, aspirin, naproxen
- oral corticosteroids, injectable steroids,
- pain medications, such as gabapentin.
They may also recommend other treatments, such as
- physical therapy
- a soft cervical collar
- ice and heat application.
In some cases, doctors may recommend surgery to treat the cause of the nerve compression. Some surgical procedures include repairing a herniated disc, widening the spinal canal space, removing a bone spur, or fusing the bones.
What if Lumbar Radiculopathy is left untreated?
The longer a person leaves radiculopathy untreated, the higher the risk is for their damage and symptoms to become permanent. In fact, in severe cases, paralysis may occur if radiculopathy is left untreated for an extended period. Radiculopathy symptoms include pain that feels like a burning sensation, numbness, and tingling in the arms or legs. If the condition is left untreated and allowed to progress, it is possible that different symptoms such as muscle weakness and muscular atrophy will begin to be seen.
Preventing radiculopathy
Some strategies may avoid compression nerve pain. These include:
- maintaining good posture, even when driving
- proper lifting techniques.
- performing regulate techniques physical activity
- developing core strength
- maintaining a moderate weight
- stretching regularly
Conclusion
ASAP Rehab and Performance, we understand how debilitating lumbar radiculopathy can be, which is why we offer a variety of treatment options to help our patients find relief. Our team of chiropractors and physical therapists work together to provide personalized care, including exercises and physical therapy, near Houston. If you are suffering from lumbar radiculopathy, we encourage you to visit us today to schedule an appointment and start your journey to recovery.